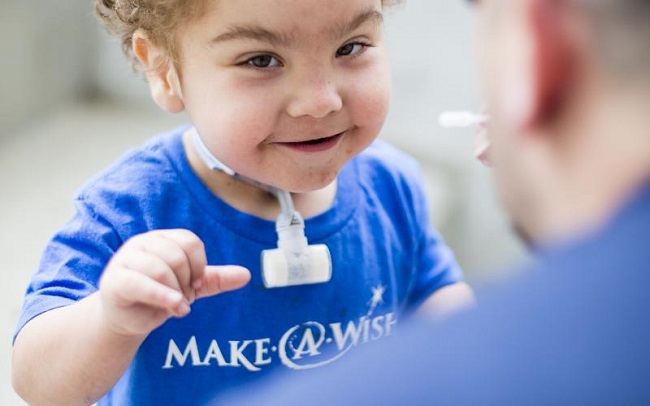
Baby Kaiba Gionfriddo has a rare condition that caused one of his lungs’ airways to collapse on exhalation. The condition led him to stop breathing and become blue when he was just 6 weeks old. Even with a mechanical ventilator, Kaiba stopped breathing practically every day, necessitating doctors to perform emergency resuscitations.
Co-author and Kaiba’s doctor, associate professor of otolaryngology Glenn Green, explains, “We’d recently had a child in the hospital who died of this, and I said, ‘there has got to be a solution that we can discover for these kids.'”
Contents
So Green and his Michigan Colleagues Attempted Something Fresh.
Using a 3-D printer, they custom-built a tiny, flexible splint that will grow with Kaiba. Professor of biomedical and mechanical engineering and co-author Scott Hollister explains that the substance utilised to repair Kaiba’s leg was created specifically to be metabolised by his body in that time frame.
Instead of producing a cast of Kaiba’s airway using plaster, they used a CT scanning, which provided them a 3-D blueprint.
Read Also:
- ERP Software
- Encryption Software
- Green Screen Software
- DK Metcalf Learns Football Speed Doesnt Equal Track Speed
- Fifa President Accused of Masterminding European Super League …
The C-shaped splint is flexible like a vacuum cleaner hose, allowing it to move with Kaiba’s breathing. Yet, Green claims that it is sturdy enough to keep his air tube from collapsing.
Kaiba’s operation in February 2012 was successful, and he was able to wean off the ventilator three weeks later. We expect this to be a permanent solution for him,” Green explains. “The splint will go away and the process will be done.”
According to Green, the porous splint is crafted from the same material as dissolveable stitches. Just as a wisteria vine grows through a trellis, Kaiba’s body will develop new cells to permeate the scaffold. Doctors are hoping that by the time the splint is entirely absorbed, Kaiba’s own tissue will be strong enough to keep his airway open.
According to Green, Kaiba will be of sufficient size at that time to tolerate a moderate constriction of the bronchi. Even a small amount of collapsing could entirely restrict air flow in a newborn’s bronchus.
Kaiba was born with tracheobronchomalaci, a disease that affects about one in 2,200 newborns. At age 2 or 3, most children outgrow it.
The tracheostomy tube that April Gionfriddo of Youngstown, Ohio claims her 19-month-old son, Kaiba, uses to get air into his windpipe is no longer causing him any problems with breathing.
Kaiba has dealt with a number of complex health issues, including a hernia, asthma, and anatomic anomalies in a number of blood arteries, so his doctor Gionfriddo is “relieved and thrilled” that he is no longer going blue. Hydrocephalus, in which fluid pushes on the brain, was also surgically corrected.
Many other Surgeons Remarked on the Michigan Group’s Creativity.
“It’s incredibly exciting,” says Sidhu Gangadharan, chief of thoracic surgery at Boston’s Beth Israel Deaconess Medical Center but not involved in Kaiba’s treatment. They encountered a one-of-a-kind challenge, and the answer they devised was equally novel.
According to Gangadharan, his hospital is likely to adopt the researchers’ practise of using 3-D printers for the creation of bespoke medical devices. Kaiba’s life was in imminent danger, therefore the FDA gave the doctors permission to mass create the gadget immediately.
According to Hollister, the 3-D printer facilitated rapid prototyping of the splint by medical professionals. These printers have functionality similar to that of inkjet printers. A biopolymer is used in place of ink as the printer deposits successive layers.
In order to make more splints for youngsters whose condition isn’t life-threatening, doctors are preparing a clinical trial.
According to Hollister, the same method might be used to create a wide range of implants, including replacement facial bones. Based on patient scans, he and Green have already constructed ears and noses, albeit they haven’t been implanted into humans just yet.
Anthony Atala, director of the Wake Forest Institute for Regenerative Medicine in North Carolina, says that researchers are already utilising 3-D printers to create scaffolds for tissue engineering with the goal of creating blood arteries and other replacement body parts.
Atala employs a 3-D printer to put down a cell-filled gel, layer by layer. Atala explains that the gel acts as a scaffold to keep the cells intact during printing. There are nutrients in the gel that the cells can use to multiply.
Read Also:
- DAW Software
- Trump will Return to Spotlight with Appearance at CPAC
- Kamala Harriss Allies Express Concern is She an Afterthought
Atala suggests that these artificial blood vessels, which have only been tried out on animals so far, could be utilised in bypass operations. They might also be utilised to supply patients undergoing kidney dialysis with blood vessels or to replace blood vessels that have been obstructed in the legs. Tissue engineering has also been employed by Atala to develop functional bladders for patients.
These methods are also being used to create cartilage-based organs including ears and tracheas by researchers. Recently, scientists at Princeton University utilised a 3-D printer to design and fabricate a bionic ear.
A new windpipe generated from stem cells implanted on a plastic scaffold was successfully transplanted into a 2-year-old girl at the University of Illinois in Peoria in April.